
Patient safety is always a priority especially during their encounter with the hospital. The Joint Commission mandates hospitals “improve the effectiveness of communication among caregivers including reporting critical results and diagnoses on a timely basis as one of the hospital’s National Patient Safety Goals” (The Joint Commission, 2018).
In Interventional Radiology (IR), we use handoff sheets when prepping both inpatients and outpatients for procedures. Outpatient pre-instruction and handoff sheets are made by procedure room nurses, and inpatient handoff sheets are made by nurses in the Radiology Patient Care Unit (RPCU). For outpatient procedures if there are no labs within 45 days prior, procedure room nurses call the referring physician’s office to arrange for labs. Handoff sheets are often written a few days prior to procedure day. With high patient turnover in IR, some patient’s relevant information such as labs is often missing or not up-to-date which includes patients holding anticoagulation medication per IR guidelines. This causes procedure delays or rescheduling since most IR procedures have a high risk for bleeding.
Literature review suggests most sentinel events in patent care occur during patient care handoffs, especially for those undergoing surgeries or procedures due to multiple checkpoints (Criscitelli, 2013). Based on these studies, bedside handoff report offers a patient-centered approach to promote patient safety (Ferguson & Howell, 2015). Therefore, I implemented a patient safety project to improve handoff report between nurses in the Radiology Prep Area and the procedure rooms when patient care is being transferred between these two areas.
An audit of handoff sheets and bedside handoff report was completed on 20 patients, selected randomly in January 2018. Questions in the audit included: 1. Does the patient have lab results written on the handoff sheet? 2. Are lab results up-to-date? 3. Are they within normal range? 4. Does the patient take anticoagulants? 5. If so, was it written on the handoff sheet and held according to IR guidelines? 6. Are these questions communicated at bedside report?
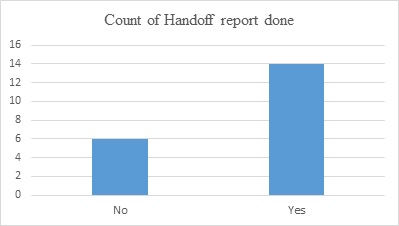
The audit showed six out of 20 patients did not have lab results written on the handoff sheets. This includes one outpatient who then had labs drawn and waited in the prep area for the results, leading to a procedure delay. Fourteen out of 20 handoff sheets were complete and patient report performed at bedside; hence 70% of handoff reports were performed correctly (see Appendix A).
To implement my patient safety project, I made a poster with power point slides and handouts. The poster was then placed in the medication room in IR. An in-service was also implemented for nurses using written handouts and anticoagulation guidelines made by our IR section chief for reference. These guidelines were posted at each nursing station so nurses have easy access when prepping patients. Evidence from literature suggests that a guiding coalition can motivate a group to embrace the change and achieve the goal of that change (Small et al., 2016). Therefore, super users for nurses were identified in the prep area and procedure rooms. They were teamed up to assist peers with queries regarding labs or medications.
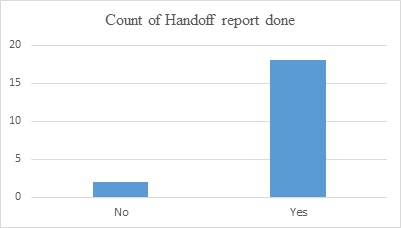
Two weeks after I implemented the in-service and placed the poster, an audit of handoff sheets and handoff report for 20 patients was performed. This showed that one patient’s lab was not up-to-date and another patient’s lab was abnormal, neither of which were discussed at bedside handoff report. Eighteen out of 20 handoff sheets were complete with lab results and anticoagulants held appropriately; hence 90% were performed correctly (see Appendix B). In this instance my project likely improved patient safety from 70% to 90%. However, our goal is to achieve 100% compliance since IR procedures are invasive with high risk for bleeding. Patient safety should always be our priority.
To achieve that goal, my project has to be sustainable. I plan to do chart audits for confirmation and also give nurses positive feedback to encourage them. I expect patient safety will improve as nursing staff share the same vision; to treat patients as our own and make safety our priority. I also plan on discussing the pros and cons with my colleagues in staff meetings to achieve our 100% adherence goal.
Appendix A
Patient hand off report is complete before patient safety project
Appendix B
Patient hand off report is complete after patient safety project
Reference
Criscitelli, T. (2013). Safe patient hand-off strategies. AORN Journal. 97(5), 582-585.
Ferguson, T., & Howell, T. (2015). Bedside reporting: protocols for improving patient care.
Burs Clin N Am, 50, 735-747.
Small, A., Gist, D., Souza, D., Dalton, J., Magny-Normilus, C., & David, D. (2016). Using Kotter’s Change Model for implementing bedside handoff. J Nurs Care Qual, 31(4), 304-309.
The Joint Commission. (2018). National patient safety goals effective January 2018.
Retrieved from https://www.jointcommission.org/standards_information/npsgs.aspx